Fatty Liver stages - Types, symptoms, causes, and treatment options

Fatty liver disease is very common, but most people don’t know they have it. In many cases, it’s picked up accidentally during an ultrasound done for a routine checkup or unrelated symptoms.
Terms like mild hepatomegaly with fatty liver, grade 1 fatty infiltration, or fatty liver grade 3 can sound alarming, especially when symptoms are minimal or absent.
However, understanding the stages, causes, and available fatty liver treatment options can help prevent progression and even reverse early disease.
At King’s Transplant Centre, patients frequently seek clarity about fatty liver symptoms, whether is fatty liver reversible, and what causes fatty liver disease. The good news is that early-stage fatty liver is highly manageable, and with the right intervention, many patients can restore normal liver health.
What is fatty Liver Disease?
Fatty liver disease occurs when excess fat accumulates inside liver cells. A healthy liver contains minimal fat, but when fat exceeds 5-10% of liver weight, it is considered fatty liver.
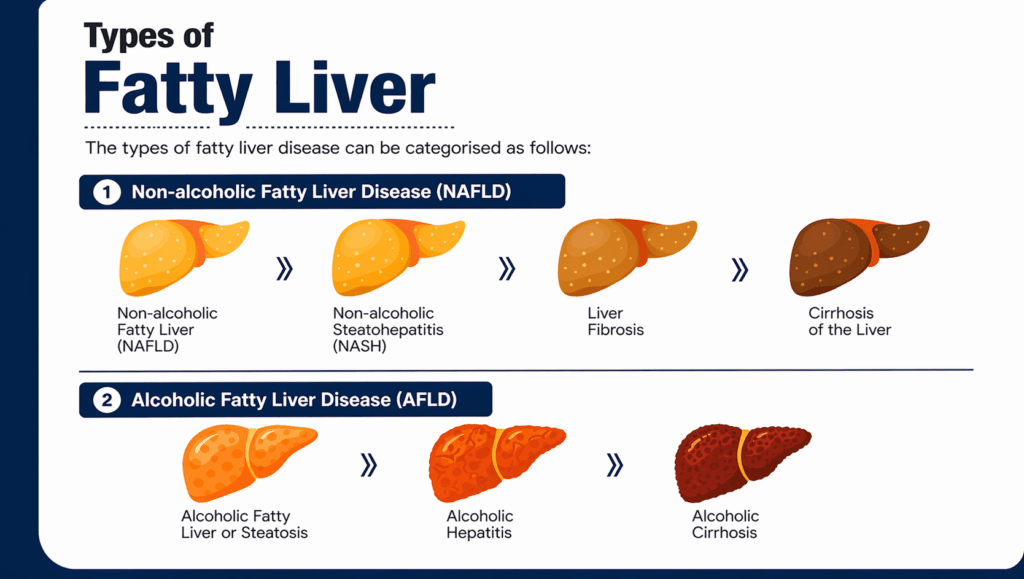
Types of Fatty Liver Disease
Fatty liver disease is classified based on its cause. Understanding the type helps determine the right fatty liver treatment, risk of progression, and whether is fatty liver reversible.
1. Non-Alcoholic Fatty Liver Disease (NAFLD)
This is the most common type and occurs in people who drink little or no alcohol. It develops due to obesity, diabetes, insulin resistance, high cholesterol, and a sedentary lifestyle. Fat gradually accumulates in liver cells and may appear on scans as mild hepatomegaly with fatty liver.
NAFLD includes two forms:
Simple Fatty Liver (Steatosis)
This is the early stage with fat accumulation but minimal inflammation.
- Usually no symptoms
- Liver function remains normal
- Completely reversible
- Often seen as mild hepatomegaly with grade 1 fatty infiltration
This stage responds well to grade 1 fatty liver treatment.
Non-Alcoholic Steatohepatitis (NASH)
This is a more advanced form where fat causes inflammation and liver damage.
- Fatigue and abdominal discomfort
- Elevated liver enzymes
- Risk of fibrosis and fatty liver grade 3
- Requires medical monitoring
2. Alcohol-related Fatty Liver Disease
Drinking too much alcohol over time can cause this type of fatty liver. The liver focuses on breaking down alcohol first, which leads to fat building up inside liver cells.
Common features:
- Enlarged liver
- Fatigue
- Mild abdominal discomfort
- Elevated liver enzymes
Stopping alcohol early can reverse this type and improve fatty liver symptoms.
3. Metabolic Fatty Liver Disease
This type is strongly linked to metabolic conditions such as:
- Obesity
- Diabetes
- High cholesterol
- High blood pressure
- Insulin resistance
It develops gradually and is commonly associated with Grade 2 fatty liver. Lifestyle changes help how to reverse fatty liver grade 2 effectively.
4. Secondary Fatty Liver
This develops due to other causes such as:
- Certain medications
- Rapid weight loss
- Malnutrition
- Hormonal disorders
- Genetic conditions
Treatment focuses on correcting the underlying cause.
Globally, studies estimate that nearly 25% of adults have fatty liver disease, and the numbers continue to rise with increasing obesity, diabetes, and sedentary lifestyles. Early detection and structured treatment remain the most effective ways to prevent complications. |
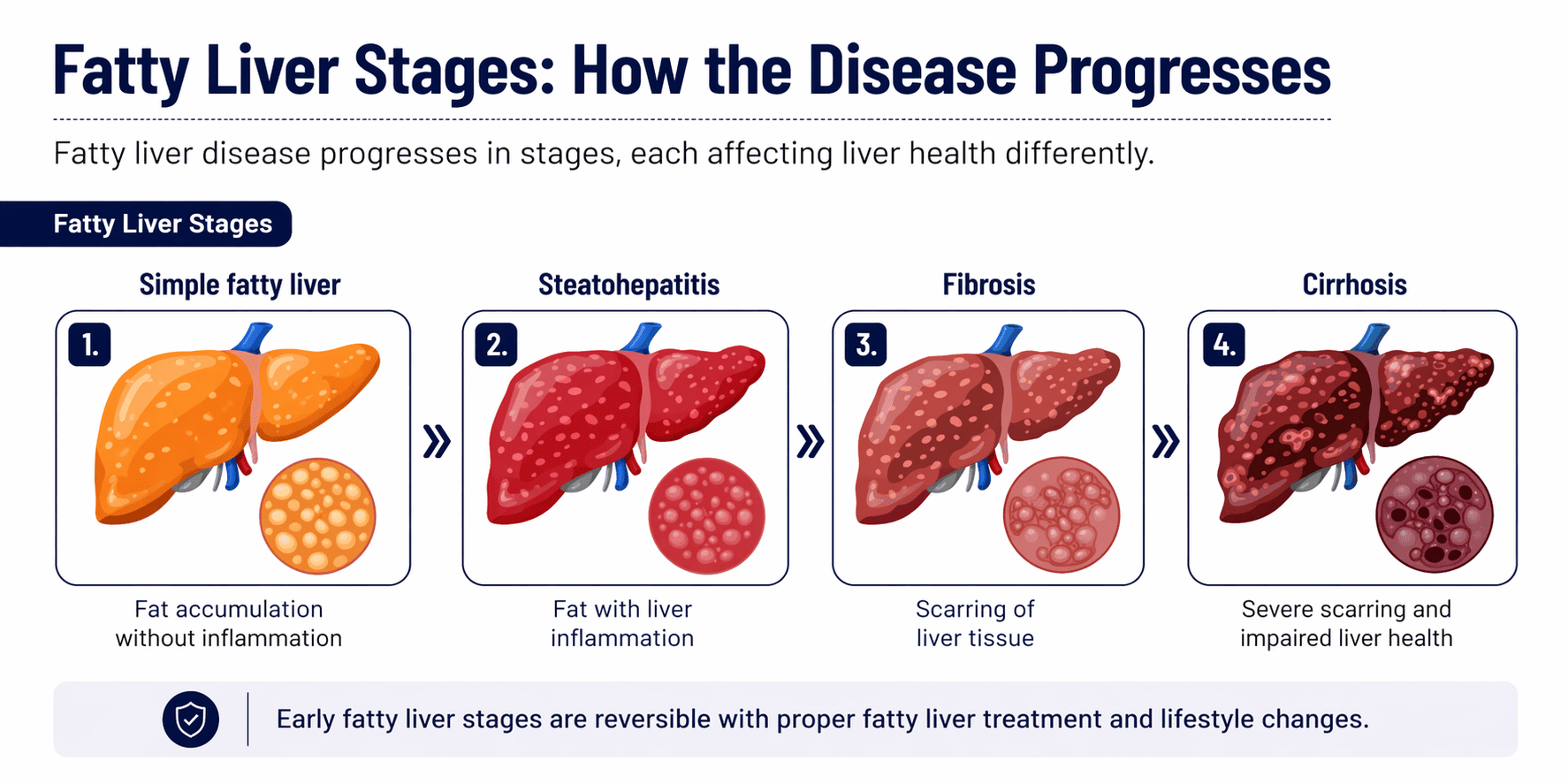
Fatty Liver stages: From mild to severe
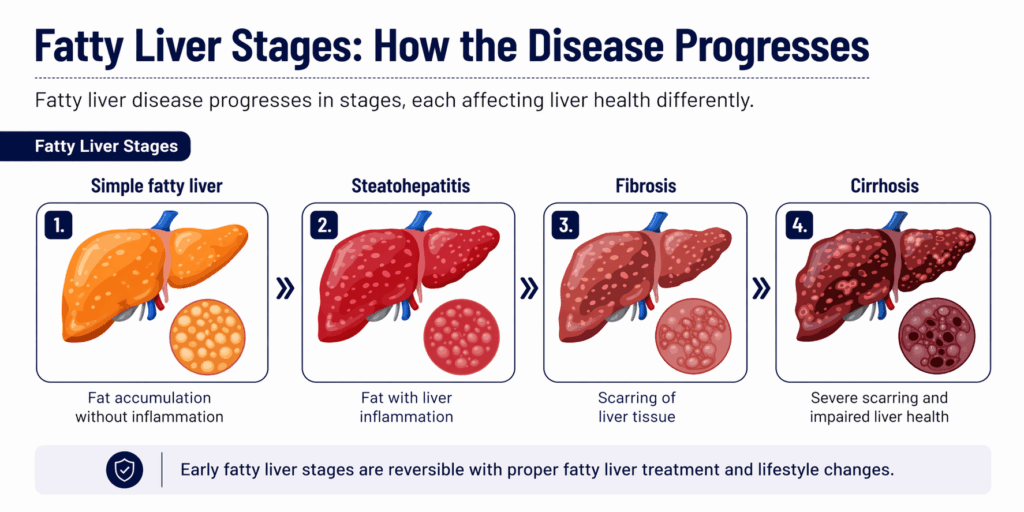
Fatty liver disease progresses gradually. Knowing these stages helps patients understand whether is grade 3 fatty liver dangerous and when treatment is urgent.
Stage 1 – Grade 1 Fatty Liver (Simple steatosis)
This is the earliest stage where fat accumulates in liver cells without inflammation or scarring.
Common features:
- Often reported as mild hepatomegaly with grade 1 fatty infiltration
- No significant symptoms
- Normal liver function
- Completely reversible
This stage responds well to grade 1 fatty liver treatment such as diet and exercise.
Stage 2 – Grade 2 Fatty Liver (Moderate fat accumulation)
Fat accumulation increases, and mild inflammation may begin.
Symptoms may include:
- Fatigue
- Mild abdominal discomfort
- Heaviness after meals
- Slightly enlarged liver
- Mild elevation in liver enzymes
Some patients may experience discomfort in the fatty liver pain area, usually on the right side of the abdomen.
This stage is still reversible, and many patients ask how to reduce fatty liver grade 2. Early lifestyle intervention is highly effective.
Stage 3 – Grade 3 fatty liver (Advanced fatty liver with fibrosis)
This is a more serious stage where inflammation leads to scar tissue formation.
Symptoms may include:
- Persistent fatigue
- Abdominal heaviness
- Nausea
- Loss of appetite
- Enlarged liver
- Digestive discomfort
This stage is commonly called fatty liver grade 3, and patients often ask is grade 3 fatty liver dangerous. At this stage, the risk of long-term liver damage increases, but progression can still be slowed with treatment.
Stage 4 – Cirrhosis (Severe liver damage)
This is the most advanced stage, where extensive scarring affects liver function.
Symptoms include:
- Jaundice
- Fluid accumulation in the abdomen
- Swelling in the legs
- Easy bruising
- Weakness
- Confusion
This stage may require advanced liver care and transplant evaluation.
Fatty Liver symptoms: What patients should watch for
One challenge with fatty liver is that fatty liver symptoms may be mild or absent, especially in early stages.
Early signs of Fatty Liver
- Fatigue
- Feeling of fullness
- Mild abdominal discomfort
- Bloating
- Weakness
- Mild enlargement of the liver
- Abnormal liver blood tests
- Signs of fatty liver are seen in an ultrasound
Many patients ask does fatty liver cause pain. Pain is usually mild and dull rather than sharp.
Advanced symptoms
- Persistent right-sided abdominal pain
- Nausea
- Poor appetite
- Weight loss
- Yellowing of skin
- Swelling in the abdomen
- Enlarged liver
Fatty Liver pain area
Pain from fatty liver is usually located:
- Right upper abdomen
- Below the rib cage
- Sometimes radiating to the back
- Dull or pressure-like sensation
This discomfort is due to liver enlargement, stretching the liver capsule.
What causes Fatty Liver Disease?
Understanding causes of fatty liver disease is important for prevention and treatment.
Metabolic causes
- Obesity
- Type 2 diabetes
- High cholesterol
- Insulin resistance
- Metabolic syndrome
Lifestyle causes
- Sedentary lifestyle
- High sugar intake
- Processed food consumption
- High refined carbohydrates
- Poor sleep
Medical conditions
- PCOS
- Hypothyroidism
- Sleep apnea
- Hormonal imbalance
Other causes
- Rapid weight loss
- Certain medications
- Genetics
- Malnutrition
Patients often ask is fatty liver dangerous; the risk depends on stage and associated conditions.
How is Fatty Liver diagnosed?
Doctors use clinical evaluation, blood tests, and imaging.
Blood tests
- ALT and AST
- Liver function tests
- Lipid profile
- Blood sugar
Imaging tests
- Ultrasound (most common)
- CT scan
- MRI
Reports may show:
- Fat infiltration
- Enlarged liver
- Mild hepatomegaly with fatty liver
Advanced diagnostic tests
- Fibroscan
- Elastography
- Liver biopsy (selected cases)
These help determine how is fatty liver diagnosed and stage severity.
Is Fatty Liver reversible?
Many patients ask is fatty liver reversible. The answer depends on stage.
- Grade 1 → Completely reversible
- Grade 2 → Reversible with treatment
- Grade 3 → Partially reversible
- Cirrhosis → Not reversible but manageable
Early fatty liver treatment provides the best outcomes.
Fatty Liver treatment options
Treatment depends on stage, underlying cause, and overall health.
Lifestyle-based Fatty Liver treatment
Weight loss is the most effective treatment.
Losing 7-10% body weight can reduce liver fat significantly.
Diet recommendations:
- Reduce sugar intake
- Avoid processed foods
- Increase vegetables
- Choose healthy fats
- Reduce refined carbs
Exercise:
- 30-45 minutes daily
- Walking
- Strength training
- Cycling
These measures help how to reverse fatty liver grade 2 naturally.
Medical treatment
Doctors may prescribe:
- Insulin resistance medications
- Vitamin E (selected patients)
- Cholesterol medications
- Liver-protective drugs
These support how to cure fatty liver when combined with lifestyle changes.
Advanced stage treatment
For fatty liver grade 3:
- Fibrosis monitoring
- Strict metabolic control
- Diabetes management
- Specialist liver care
In severe cases:
- Cirrhosis management
- Fluid control
- Portal hypertension treatment
- Liver transplant evaluation
This is where specialized care at King’s Transplant Centre becomes important.
Early detection can prevent liver damage
Fatty liver disease is common but manageable when detected early. From grade 1 fatty liver treatment to management of fatty liver grade 3, timely lifestyle changes and medical care can prevent progression. Recognizing fatty liver symptoms, understanding what causes fatty liver disease, and knowing how is fatty liver diagnosed helps patients take control of their liver health.
At King’s Transplant Centre, patients receive comprehensive evaluation and personalized fatty liver treatment plans designed to slow disease progression and improve liver function. With early intervention, fatty liver is often reversible, and long-term liver damage can be avoided.
FAQs
Fatty liver is not dangerous in early stages, but may lead to fibrosis and cirrhosis if untreated.
Yes, fatty liver may cause dull pain in the right upper abdomen, known as the fatty liver pain area.
Weight loss, a healthy diet, exercise, and diabetes control can reverse grade 2 fatty liver.
Yes, grade 3 fatty liver indicates fibrosis and increases the risk of liver damage.
Fatty liver is diagnosed using blood tests, ultrasound, Fibroscan, and sometimes MRI.
Overview
When to consult a liver specialist?
You should consult a liver specialist if fatty liver is detected on imaging or if symptoms persist. Early evaluation helps prevent progression to advanced stages like fibrosis or fatty liver grade 3.
Seek medical advice at King’s Transplant Centre if you experience:
- Persistent fatigue or weakness
- Dull pain or heaviness in the right upper abdomen
- Abnormal liver function tests
- Diabetes, obesity, or high cholesterol with fatty liver
- Ultrasound showing fatty liver or liver enlargement
- Reports mentioning mild hepatomegaly with fatty liver
- Unexplained appetite or weight changes
- Family history of liver disease
The specialists at King’s Transplant Centre may recommend further evaluation such as Fibroscan, detailed blood tests, and personalized fatty liver treatment to monitor progression and protect long-term liver health.