Pediatric Liver Transplant vs Adult Liver Transplant

When a child is diagnosed with severe liver disease, parents are suddenly faced with decisions they never expected to make. Questions around survival, recovery, and long-term health become urgent. In many such cases, a pediatric liver transplant is not just a treatment option—it becomes a lifeline.
At specialized centres like King’s Transplant Centre, families are guided through this complex journey with expertise and compassion. But it’s important to understand that a child liver transplant is not simply a smaller version of adult surgery. It is a highly specialised procedure designed around the unique needs of growing bodies and developing systems.
What is Pediatric Liver Transplant?
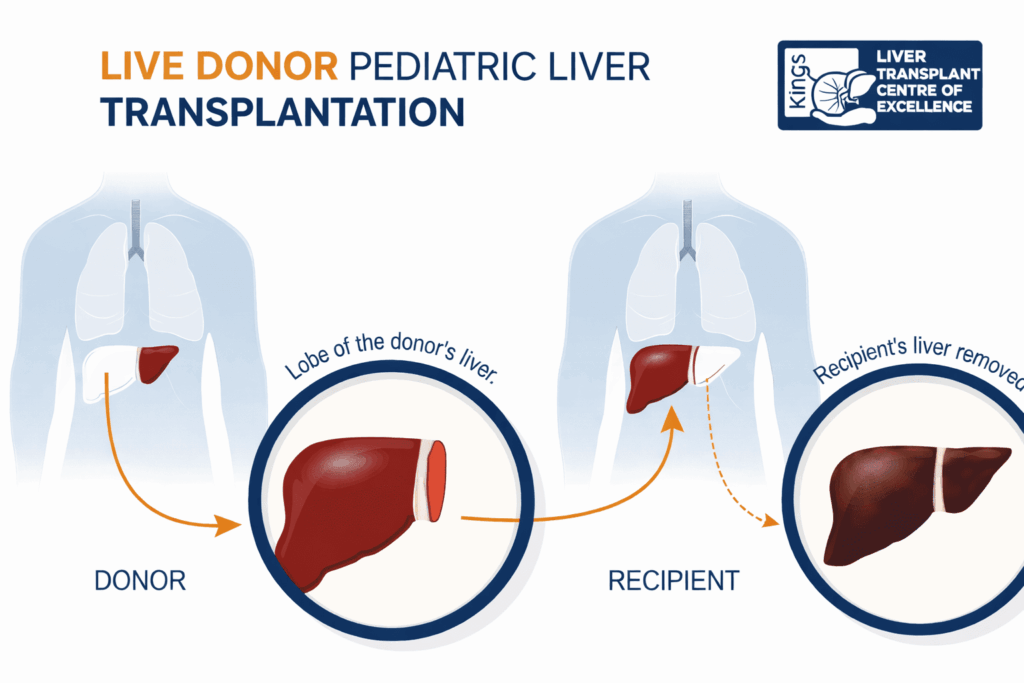
A pediatric liver transplant is a surgical procedure where a diseased or failing liver in a child is replaced with a healthy liver (or a segment of one) from a donor.
Unlike adults, children—especially those undergoing an infant liver transplant—often receive a portion of a liver rather than a whole organ. This is possible because the liver has the remarkable ability to regenerate and grow with the child.
This procedure is carefully planned to:
- Restore normal liver function
- Support growth and development
- Prevent life-threatening complications
For many families, understanding what is liver transplant in children helps reduce fear and allows them to make informed decisions.
Why children need a transplant and why it’s different
Unlike adults, where liver failure often comes from years of disease, unhealthy habits, or age-related damage, children often need transplantation because of conditions present at birth or developed early in life. Common causes include congenital abnormalities, metabolic disorders, or acute liver failure.
For instance, in infants and young children, issues like blocked or malformed bile ducts, genetic/metabolic liver diseases, or sudden, severe liver failure can make a liver transplant the only viable treatment.
Because children’s bodies are still growing, the goal is not only to replace a failed organ but to restore growth, development, and a whole, healthy life. That means transplant isn’t just about survival: it’s about giving a child a future.
What makes pediatric transplants more complex
Operating on a child’s body presents very different challenges compared with adults:
- Blood vessels and bile ducts are tiny. In an infant, veins or ducts may be only a few millimetres; stitching them under microsurgical magnification demands extreme precision.
- The graft (donated liver segment) must be carefully sized. If the portion is too large, it can press on other organs; too small, and it might fail to support growth.
- Bile duct reconstruction is more delicate, and risks like bile leaks or strictures are higher.
- Anesthesia and intensive post-op care must be adjusted for a child’s physiology, requiring a specialized pediatric transplant team.
These challenges mean that not every hospital or transplant center is equipped for pediatric liver transplantation. That’s why a centre like King’s Transplant Centre, which offers dedicated Paediatric Liver Transplant services, becomes so vital.

Recovery and long-term life: What to expect
After a child’s liver transplant, most kids experience a massive improvement in their health. Signs of liver failure ease, their growth gets back on track, and they start enjoying life again. Children who were once very sick, underweight, or delayed in their development can go back to school, play with friends, and grow just like other kids their age.
Many parents understandably ask: “Is liver transplant safe?” With modern surgical techniques and the expertise of teams like those at King’s Transplant Centre, pediatric liver transplants are now safer than ever. Success rates are high, and serious complications are relatively rare.
Even so, a pediatric liver transplant is just the start of lifelong care. Children need regular check-ups, medications to prevent organ rejection, and close monitoring as they grow. With proper follow-up, children can lead active, healthy lives and enjoy a future full of possibilities after their transplant.
Who Can Donate a Liver to a Child?
The criteria governing who can give and who can receive a liver for a child are quite specific, prioritizing safety and size matching.
Understanding the donor
- Donor Age: Individuals donating liver segments for pediatric patients are almost exclusively adults, frequently the child’s parents or other immediate close family members.
- Safety & Size: A crucial constraint is the absolute need to maintain the donor’s safety. For this reason, and due to the physiological challenges of segment sizing, very young or small children are typically not considered as donors. The risk-benefit calculation makes them ineligible.
- Key Consideration: Successful segment transplantation relies heavily on matching the size of the liver portion to the recipient’s body cavity and ensuring the remaining liver is adequate for the donor.
Understanding the recipient
- Recipient Age Range: The patients undergoing these procedures generally span from infants and children to, in certain medically necessary cases, teenagers.
- Governing Factors: Eligibility is determined not just by age, but critically by the severity of the child’s underlying condition (e.g., biliary atresia, metabolic disorders) and the specific internal policies of the transplant center.
Infant Liver Transplant: Unique Challenges
Performing an infant liver transplant is among the most delicate procedures in modern surgery.
Challenges include:
- Extremely small blood vessels
- Higher risk of complications
- Difficulty in size-matching donor liver
- Specialized anesthesia requirements
Even minor surgical variations can significantly impact outcomes. That’s why infant liver transplant procedures are typically carried out in highly specialised centres with experienced pediatric transplant teams. Centres such as King’s Transplant Centre, with dedicated pediatric expertise and multidisciplinary care, are equipped to handle these complex cases with precision and continuity of care.
Differences Between Pediatric and Adult Liver Transplants
In most cases, the donor is the child’s mother or father. Children only need a small part of the liver, so a parent can safely donate a portion. The donated liver and the remaining liver in the parent both grow back over time. This is one of the biggest differences in pediatric liver transplant vs adult liver transplant
Key differences:
| Factor | Pediatric Liver Transplant | Adult Liver Transplant |
|---|---|---|
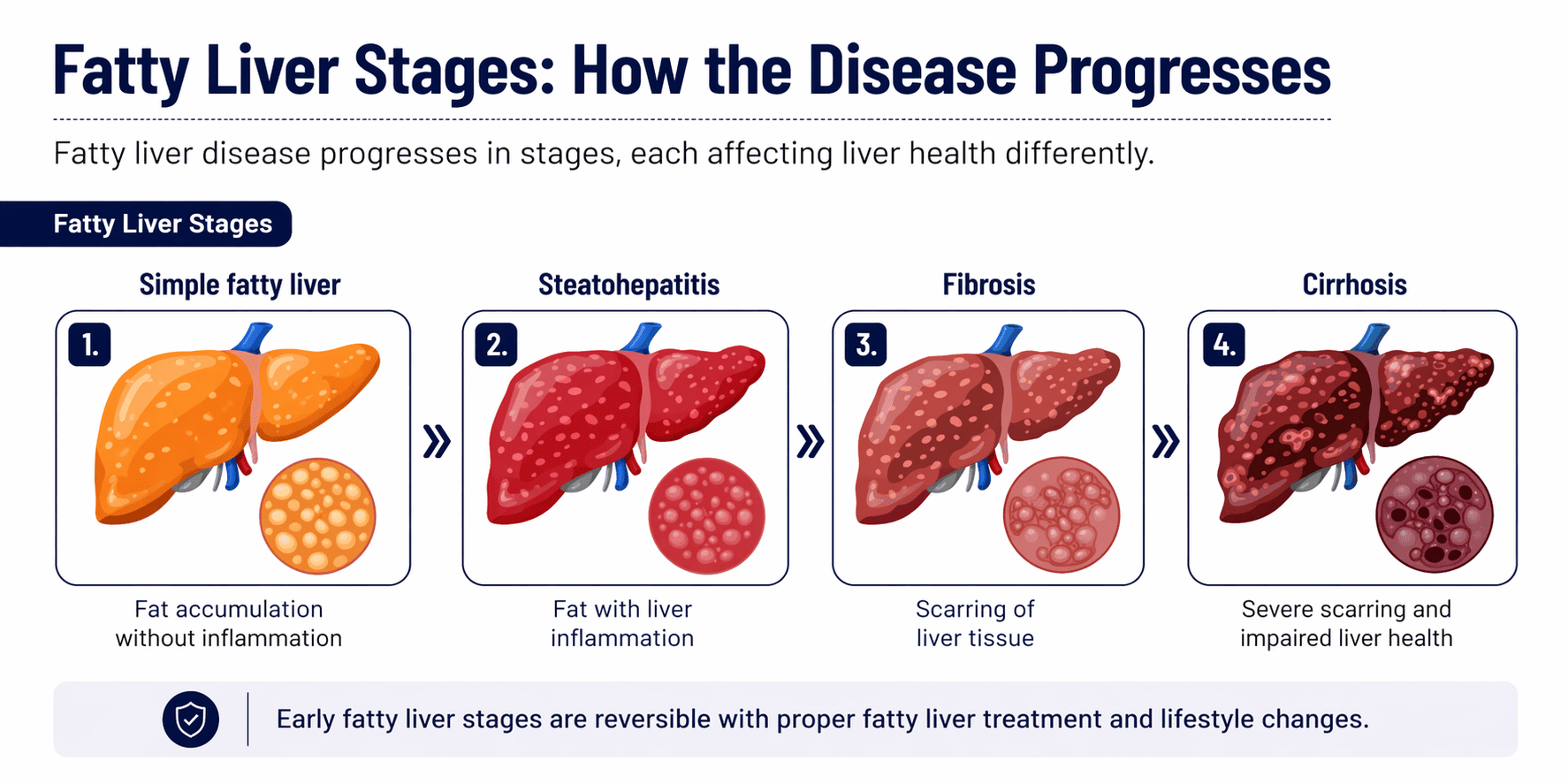
| Main cause | Biliary atresia, genetic disease | Cirrhosis, fatty liver, alcohol |
| Donor | Usually parent | Usually deceased donor |
| Liver used | Small liver segment | Whole liver or larger segment |
| Surgery | Microsurgery because vessels are tiny | Standard surgery |
| Recovery | Faster | Slower |
| Goal | Growth and normal development | Restore liver function |
| Hospital stay | Usually shorter | Usually longer |
| Long-term care | Growth and nutrition monitoring | Disease and lifestyle management |
Understanding what is liver transplant in both contexts highlights why children need a completely different approach.
Real Patient Perspective
In clinical practice, many children undergoing pediatric liver transplant initially present with poor growth, fatigue, and repeated hospital visits. After successful transplantation, parents often notice dramatic improvements—better appetite, weight gain, and increased activity.
Still, every case is unique. Some children may face complications, require re-hospitalisation, or need long-term adjustments. Ethical care involves setting realistic expectations while offering hope.
Frequently Asked Questions (FAQs)
Yes, in many cases, parents are the most common donors in a child liver transplant, as they are more likely to be compatible and available for living donor transplantation.
A pediatric liver transplant surgery usually takes between 6 to 12 hours, depending on the complexity of the case and the child’s condition.
Most children go on to live active, fulfilling lives after recovery. They can attend school, play sports, and grow normally with proper medical care.
Follow-up includes:
- Regular blood tests
- Monitoring liver function
- Medication adjustments
- Growth and developmental assessments
This ongoing care is essential for long-term success.
Doctors assess urgency based on:
- Liver function tests
- Symptoms (jaundice, swelling, fatigue)
- Risk of liver failure progression
In acute cases, an urgent pediatric liver transplant may be life-saving.
If a donor is not available, the child may be placed on a transplant waiting list. In some cases, living donor options are explored to reduce waiting time.
A liver transplant replaces the diseased liver, but it is not considered a complete “cure.” Lifelong care, monitoring, and medication are required to maintain liver health.
Liver transplant recovery for kids is often faster because children heal more efficiently. However, they require closer monitoring for growth, development, and medication adjustments over time compared to adults.
Why King’s Transplant centre stands out?
At King’s Transplant Centre, the team is trained at one of the world’s leading liver centers and offers both adult and infant liver transplant services in the same facility. They have experience with living-donor transplants, split (cadaveric) liver transplants, and smaller grafts explicitly designed for children.
The center provides a full, multidisciplinary care team of surgeons, pediatric anesthetists, intensivists, hepatologists, and support staff, all familiar with the special needs of children and their families.
With their strong international reputation, patient-focused care, and excellent success rates, King’s Transplant Centre is a trusted choice for families seeking a child liver transplant.
Overview
Get a second opinion for your child’s liver condition
A child liver transplant is more than a surgery; it’s a chance for a new life. It demands deep expertise, careful planning, and long-term commitment. But for many children, it means growing up, playing, studying, and dreaming just like any other healthy child.
If you’re considering a pediatric liver transplant, infant liver transplant, or want to learn if transplant is the best option for your child, reach out to experienced centres such as King’s Transplant Centre. With proper care and monitoring, a transplant can bring hope, health, and a future.
Because when it comes to giving a child a second chance at life, precision, compassion, and expertise truly matter.
Medical Disclaimer
This content is for informational purposes only and does not replace professional medical advice, diagnosis, or treatment. Every child’s condition is unique. Always consult a qualified pediatric hepatologist or transplant specialist before making medical decisions.